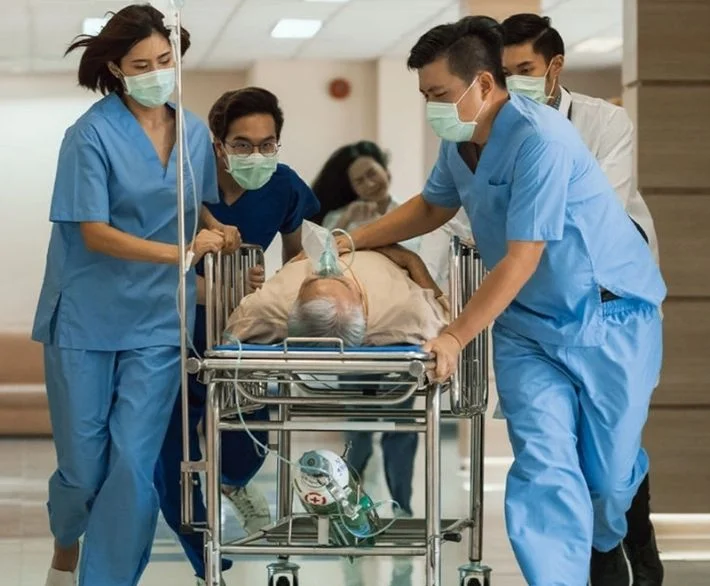
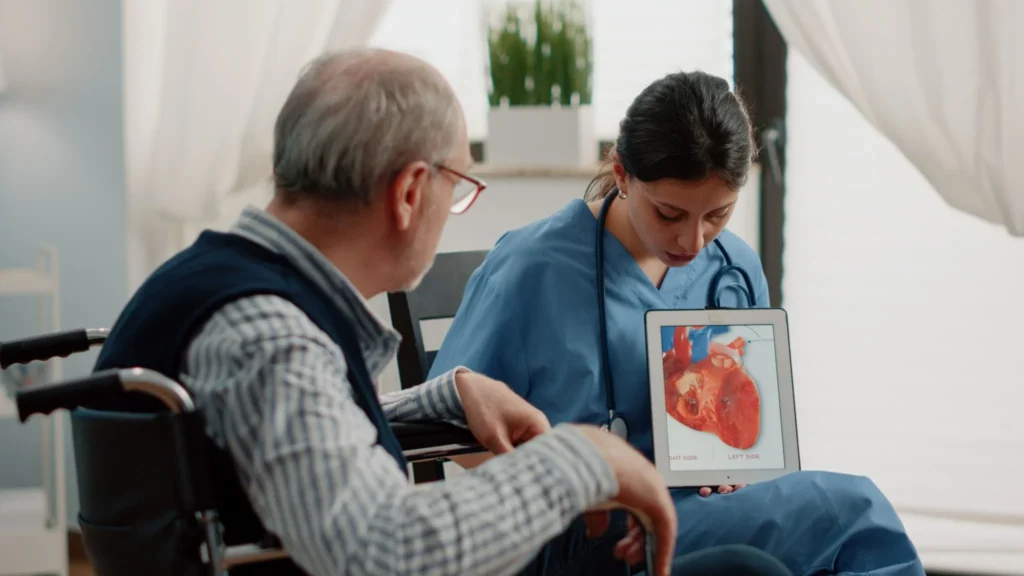
Delivering Precision, Compassion, and 24/7 Critical Care Excellence
Critical care medicine is not just a specialty — it is a responsibility that demands vigilance, precision, teamwork, and unwavering commitment. As an Intensivist, I dedicate myself to providing round-the-clock, evidence-based, and patient-centered care to those who need it most. About Critical Care Medicine The Department of Critical Care manages patients with life-threatening conditions requiring advanced monitoring, organ support, and rapid intervention. This includes patients with severe infections, respiratory failure, cardiac emergencies, trauma, multi-organ dysfunction, and post-operative complications. Modern critical care is dynamic and technology-driven. From advanced ventilatory strategies and hemodynamic monitoring to bedside ultrasound and protocol-based resuscitation, our ICU functions as a highly coordinated ecosystem where every second matters. But beyond technology, critical care is about judgment, timing, and human connection — supporting families through uncertainty while making complex decisions with clarity and compassion. My Approach as an Intensivist Critical care revolves around three core principles: 1. Evidence-Based Precision I believe in delivering care grounded in updated scientific evidence and best clinical practices. Every intervention — whether mechanical ventilation, vasopressor support, or antimicrobial therapy — must be individualized and thoughtfully applied. 2. Dynamic and Adaptive Management Critical illness evolves rapidly. My approach emphasizes continuous reassessment, early recognition of deterioration, and proactive decision-making. The ICU is not static; it demands constant vigilance and flexibility. 3. Compassionate Communication Families experience immense stress when a loved one is critically ill. Transparent communication, realistic discussions, and emotional support are integral components of my practice. Medicine must be humane, especially in moments of vulnerability. Bridging the Gaps in Critical Care One of my key visions is to strengthen the bridge between emergency stabilization and definitive recovery by: My goal is to reduce preventable complications, optimize outcomes, and elevate the standard of care delivered in our ICU. 24/7 Commitment Critical illness does not follow a schedule. My availability reflects my commitment to immediate assessment and timely intervention whenever needed. Continuity of care is crucial in critical care medicine, and I strive to ensure that every patient receives consistent, high-quality management at all hours. In critical care, every decision matters. Every minute counts. Every patient deserves our absolute best. Through precision, vigilance, and compassion, I remain dedicated to delivering comprehensive and dynamic critical care for those entrusted to us.